Volume 34, Issue 2 (7-2025)
JGUMS 2025, 34(2): 180-191 |
Back to browse issues page
Research code: ۱۴۰۱۰۸۰۹۰۲
Ethics code: IR.GUMS.REC.1402.056
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Monfared A, Rimaz S, Anvari S, Panahi L, Ghazanfar Tehran S, Pouy S, et al . Frequency of Organ Donation and the Related Factors in Patients With Low Consciousness Level Below 5 Admitted to Hospitals in Guilan Province, Iran. JGUMS 2025; 34 (2) :180-191
URL: http://journal.gums.ac.ir/article-1-2717-en.html
URL: http://journal.gums.ac.ir/article-1-2717-en.html
Ali Monfared1 
 , Siamak Rimaz2
, Siamak Rimaz2 
 , Saeid Anvari1
, Saeid Anvari1 
 , Latif Panahi *3
, Latif Panahi *3 
 , Samaneh Ghazanfar Tehran1
, Samaneh Ghazanfar Tehran1 
 , Somaye Pouy4
, Somaye Pouy4 
 , Keyvan Abdi5
, Keyvan Abdi5 
 , Arezo Khiali5
, Arezo Khiali5 
 , Morteza Rahbar-Taramsari6
, Morteza Rahbar-Taramsari6 
 , Saman Maroufizadeh7
, Saman Maroufizadeh7 


 , Siamak Rimaz2
, Siamak Rimaz2 
 , Saeid Anvari1
, Saeid Anvari1 
 , Latif Panahi *3
, Latif Panahi *3 
 , Samaneh Ghazanfar Tehran1
, Samaneh Ghazanfar Tehran1 
 , Somaye Pouy4
, Somaye Pouy4 
 , Keyvan Abdi5
, Keyvan Abdi5 
 , Arezo Khiali5
, Arezo Khiali5 
 , Morteza Rahbar-Taramsari6
, Morteza Rahbar-Taramsari6 
 , Saman Maroufizadeh7
, Saman Maroufizadeh7 

1- Department of Internal Medicine, Regenerative Medicine, Organ Procurement and Transplantation multidisciplinary Center, School of Medicine, Razi Hospital, Guilan University of Medical Sciences, Rasht, Iran.
2- Department of Anesthesiology, Anesthesiology Research Center, Alzahra Hospital, Guilan University of Medical Sciences, Rasht, Iran.
3- Department of Emergency and Intensive Care Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
4- Department of Pediatric Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
5- Regenerative Medicine, Organ Procurement and Transplantation Multidisciplinary Center, Razi Hospital, Guilan University of Medical Sciences, Rasht, Iran.
6- Department of Forensic Medicine, School of Medicine, Razi Hospital, Guilan University of Medical Sciences, Rasht, Iran.
7- Department of Biostatistics, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
2- Department of Anesthesiology, Anesthesiology Research Center, Alzahra Hospital, Guilan University of Medical Sciences, Rasht, Iran.
3- Department of Emergency and Intensive Care Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
4- Department of Pediatric Nursing, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
5- Regenerative Medicine, Organ Procurement and Transplantation Multidisciplinary Center, Razi Hospital, Guilan University of Medical Sciences, Rasht, Iran.
6- Department of Forensic Medicine, School of Medicine, Razi Hospital, Guilan University of Medical Sciences, Rasht, Iran.
7- Department of Biostatistics, School of Nursing and Midwifery, Guilan University of Medical Sciences, Rasht, Iran.
Full-Text [PDF 5084 kb]
(333 Downloads)
| Abstract (HTML) (1013 Views)
Full-Text: (463 Views)
Introduction
The incidence of accidents causing the occurrence of brain death in Iran is high. In this regard, the use of brain death cases’ organs for transplantation has been carried out in Iran for a long time. Several factors are influential in this field. Guilan province is the center of organ donation and transplantation in Iran. The present study aims to determine the frequency of organ donation and the related factors in patients with a low consciousness level in hospitals of Guilan province.
Methods
In this analytical cross-sectional study, the data of all patients with a Glasgow coma scale (GCS) score less than five admitted to the hospitals of Guilan province in 2021 and 2022 were examined. Information was extracted from the medical files of patients, the organ procurement unit (OPU), and the organ transplantation registry of Iran. After entering the data in SPSS software, version 21, data were analyzed using descriptive and inferential statistics.
Results
The results showed the mean age of participants was 52.06±19.9 years. There were 245 males (74.9%) and 82 females (25.1%). Most of patients were married (n=266, 81.3%). The mean BMI was 26.25±3.23. For brain death cases, the mean age was 38.26±12.9 years. The most common blood type was O+ (n=187, 57.2%) while the rarest blood type was AB- (n=8, 2.4%). Most participants had a high school diploma (33.3%), with moderate income (59.6%), and were mostly self-employed (58.7%), with no organ donation card (93.9%).
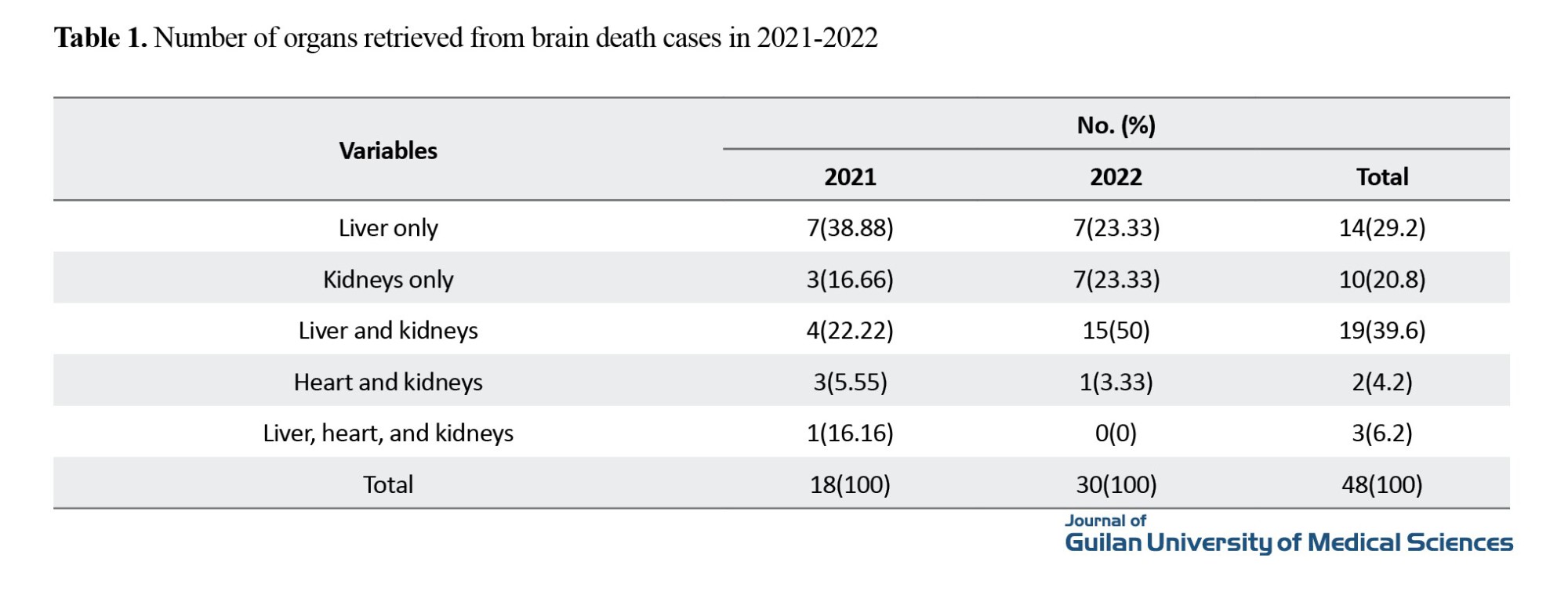
The most common reasons for not donating organs were the non-occurrence of brain death (30.9%) and not being suitable for organ donation (30%). Also, among 195 brain death cases, there were 27 cases (30.7%) whose relatives did not declare consent for organ donation. In 2021, there were 179 patients with a GCS below 5, which decreased to 148 in 2022. Among 48 brain-dead organ donors, 109 organs were retrieved for transplantation. The most commonly retrieved organs were kidneys (n=68, 62.4%), livers (n=36, 33%), and hearts (n=5, 4.6%). The number of organs retrieved from brain death cases in 2021 and 2022 is shown in Table 1.
Analysis of patient records showed that 96 patients (29.4%) had diabetes, 175(53.5%) had hypertension, 11 (3.4%) had malignancies, 56(17.1%) had heart disease, 82(25.1%) had undergone surgery, and 134(59%) had a history of smoking and alcohol use. The leading causes of decreased consciousness leading to brain death were cerebrovascular events (48.3%), trauma (37.3%), and cardiovascular events (6.1%), while malignancies (4.3%) and unknown causes (0.4%) were less frequent. Among cerebrovascular events, stroke was the most common event (n=101, 30.9%), followed by spontaneous hemorrhage (n=46, 14.1%) and cerebral vascular aneurysm (n=11, 3.4%). In trauma-related events, car/motorcycle accident was the most common event (n=95, 28.1%), followed by falling (n=27, 8.3%). Among cardiovascular events, cerebral hypoxia following CPR was the most common event (n=15, 4.6%).
Conclusion
The present study demonstrated that cerebrovascular events were the most prevalent cause of brain death in Iran, accounting for nearly half of all cases. A detailed analysis revealed that among patients with low consciousness (GCS<5), a remarkably high number had brain death. While a substantial number of these brain-dead patients met the initial criteria for organ donation, our findings indicate that approximately 40-60% of cases presented with either relative or absolute contraindications that ultimately precluded donation. Absolute contraindications included active HIV infection, COVID-19, and metastatic malignancies, while relative contraindications were higher age (>65 years), uncontrolled systemic infections (particularly septicemia), significant hemodynamic instability requiring high-dose vasopressors, and various legal impediments. Notably, the study observed that nearly 30% of potential donors were excluded due to cardiovascular events. We found that family refusal is the most significant barrier to organ donation, reported in approximately 60% of eligible cases.
We recommend implementing a multi-dimensional strategy to address these challenges: Hospital-based family education programs by trained counselors, developing nationwide public awareness campaigns to destigmatize organ donation, and creating standardized protocols for evaluating donors in critical care settings.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethics Committee of Guilan University of Medical Sciences, Rasht, Iran (Code: IR.GUMS.REC.1402.056).
Funding
This study was funded by the Multidisciplinary Center for Reconstructive Medicine, Organ Procurement and Transplantation and the Guilan University of Medical Sciences.
Authors contributions
Preparing the initial draft and acquisition, analysis, or interpretation of data: Ali Monfared, Saeid Anvari, Siamak Rimaz, Latif Panahi, Somaye Pouy and, Samaneh Ghazanfar Tehran; Study concept and design: Ali Monfared, Saeid Anvari, Siamak Rimaz and, Latif Panahi; Statistical analysis: Saman Maroufizadeh, Latif Panahi and, Somaye Pouy; Funding acquisition: Siamak Rimaz and Latif Panahi; Administrative, technical, or material support: Siamak Rimaz, Arezo Khiali, Keyvan Abdi and, Latif Panahi; Study supervision: Ali Monfared, Siamak Rimaz, Saeid Anvari, and Morteza Rahbar-Taramsari.
Conflicts of interest
The authors declare no conflict of interest.
Acknowledgments
The authors would like to thank the Multidisciplinary Center for Reconstructive Medicine, Reconstructive Organ Procurement and Transplantation, the Guilan University of Medical Sciences, the staff of Razi Hospital in Rasht, and all participants for their support and cooperation in this study.
The incidence of accidents causing the occurrence of brain death in Iran is high. In this regard, the use of brain death cases’ organs for transplantation has been carried out in Iran for a long time. Several factors are influential in this field. Guilan province is the center of organ donation and transplantation in Iran. The present study aims to determine the frequency of organ donation and the related factors in patients with a low consciousness level in hospitals of Guilan province.
Methods
In this analytical cross-sectional study, the data of all patients with a Glasgow coma scale (GCS) score less than five admitted to the hospitals of Guilan province in 2021 and 2022 were examined. Information was extracted from the medical files of patients, the organ procurement unit (OPU), and the organ transplantation registry of Iran. After entering the data in SPSS software, version 21, data were analyzed using descriptive and inferential statistics.
Results
The results showed the mean age of participants was 52.06±19.9 years. There were 245 males (74.9%) and 82 females (25.1%). Most of patients were married (n=266, 81.3%). The mean BMI was 26.25±3.23. For brain death cases, the mean age was 38.26±12.9 years. The most common blood type was O+ (n=187, 57.2%) while the rarest blood type was AB- (n=8, 2.4%). Most participants had a high school diploma (33.3%), with moderate income (59.6%), and were mostly self-employed (58.7%), with no organ donation card (93.9%).
The most common reasons for not donating organs were the non-occurrence of brain death (30.9%) and not being suitable for organ donation (30%). Also, among 195 brain death cases, there were 27 cases (30.7%) whose relatives did not declare consent for organ donation. In 2021, there were 179 patients with a GCS below 5, which decreased to 148 in 2022. Among 48 brain-dead organ donors, 109 organs were retrieved for transplantation. The most commonly retrieved organs were kidneys (n=68, 62.4%), livers (n=36, 33%), and hearts (n=5, 4.6%). The number of organs retrieved from brain death cases in 2021 and 2022 is shown in Table 1.

Analysis of patient records showed that 96 patients (29.4%) had diabetes, 175(53.5%) had hypertension, 11 (3.4%) had malignancies, 56(17.1%) had heart disease, 82(25.1%) had undergone surgery, and 134(59%) had a history of smoking and alcohol use. The leading causes of decreased consciousness leading to brain death were cerebrovascular events (48.3%), trauma (37.3%), and cardiovascular events (6.1%), while malignancies (4.3%) and unknown causes (0.4%) were less frequent. Among cerebrovascular events, stroke was the most common event (n=101, 30.9%), followed by spontaneous hemorrhage (n=46, 14.1%) and cerebral vascular aneurysm (n=11, 3.4%). In trauma-related events, car/motorcycle accident was the most common event (n=95, 28.1%), followed by falling (n=27, 8.3%). Among cardiovascular events, cerebral hypoxia following CPR was the most common event (n=15, 4.6%).
Conclusion
The present study demonstrated that cerebrovascular events were the most prevalent cause of brain death in Iran, accounting for nearly half of all cases. A detailed analysis revealed that among patients with low consciousness (GCS<5), a remarkably high number had brain death. While a substantial number of these brain-dead patients met the initial criteria for organ donation, our findings indicate that approximately 40-60% of cases presented with either relative or absolute contraindications that ultimately precluded donation. Absolute contraindications included active HIV infection, COVID-19, and metastatic malignancies, while relative contraindications were higher age (>65 years), uncontrolled systemic infections (particularly septicemia), significant hemodynamic instability requiring high-dose vasopressors, and various legal impediments. Notably, the study observed that nearly 30% of potential donors were excluded due to cardiovascular events. We found that family refusal is the most significant barrier to organ donation, reported in approximately 60% of eligible cases.
We recommend implementing a multi-dimensional strategy to address these challenges: Hospital-based family education programs by trained counselors, developing nationwide public awareness campaigns to destigmatize organ donation, and creating standardized protocols for evaluating donors in critical care settings.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethics Committee of Guilan University of Medical Sciences, Rasht, Iran (Code: IR.GUMS.REC.1402.056).
Funding
This study was funded by the Multidisciplinary Center for Reconstructive Medicine, Organ Procurement and Transplantation and the Guilan University of Medical Sciences.
Authors contributions
Preparing the initial draft and acquisition, analysis, or interpretation of data: Ali Monfared, Saeid Anvari, Siamak Rimaz, Latif Panahi, Somaye Pouy and, Samaneh Ghazanfar Tehran; Study concept and design: Ali Monfared, Saeid Anvari, Siamak Rimaz and, Latif Panahi; Statistical analysis: Saman Maroufizadeh, Latif Panahi and, Somaye Pouy; Funding acquisition: Siamak Rimaz and Latif Panahi; Administrative, technical, or material support: Siamak Rimaz, Arezo Khiali, Keyvan Abdi and, Latif Panahi; Study supervision: Ali Monfared, Siamak Rimaz, Saeid Anvari, and Morteza Rahbar-Taramsari.
Conflicts of interest
The authors declare no conflict of interest.
Acknowledgments
The authors would like to thank the Multidisciplinary Center for Reconstructive Medicine, Reconstructive Organ Procurement and Transplantation, the Guilan University of Medical Sciences, the staff of Razi Hospital in Rasht, and all participants for their support and cooperation in this study.
References
- Lewis A, Koukoura A, Tsianos GI, Gargavanis AA, Nielsen AA, Vassiliadis E. Organ donation in the US and Europe: The supply vs demand imbalance. Transplantation Reviews. 2021; 35(2):100585. [DOI:10.1016/j.trre.2020.100585] [PMID]
- Sade RM. Brain death, cardiac death, and the dead donor rule. Journal of the South Carolina Medical Association (1975). 2011; 107(4):146-9. [PMID]
- Wijdicks EF. The diagnosis of brain death. New England Journal of Medicine. 2001; 344(16):1215-21 [DOI:10.1056/NEJM200104193441606] [PMID]
- Iranian Society of Organ Donation. [Reviewing on organ donation Tehran (Persian)]. Tehran: Iranian Society of Organ Donation; 2015. [Link]
- Iranian Society of Organ Donation. [Donation (Persian)]. Tehran: Iranian Society of Organ Donation; 2022. [Link]
- Kiani M, Abbasi M, Ahmadi M, Salehi B. Organ transplantation in Iran; current state and challenges with a view on ethical consideration. Journal of Clinical Medicine. 2018; 7(3):45 [DOI:10.3390/jcm7030045] [PMID]
- Wolfe RA, Roys E, Merion RM. Trends in organ donation and transplantation in the United States, 1999-2008. American Journal of Transplantation. 2010; 10(4):961-72. [DOI:10.1111/j.1600-6143.2010.03021.x] [PMID]
- Rech TH, Moraes RB, Crispim D, Czepielewski MA, Leitao CB. Management of the brain-dead organ donor: A systematic review and meta-analysis. Transplantation. 2013; 95(7):966-74 [DOI:10.1097/TP.0b013e318283298e] [PMID]
- McQuillan KA, Makic MBF, Whalen E. Trauma nursing E-Book: From resuscitation through rehabilitation. Amsterdam: Elsevier Health Sciences; 2019. [Link]
- Manzari Z, Mohammadi E, Heydari A, Shearbaff HA, Azizi MM, Khaleghi E. Exploring the needs and perceptions of Iranian families faced with brain death news and request to donate organ: A qualitative study. International Journal of Organ Transplantation Medicine. 2012; 3(2):92. [PMID]
- Abbasi Z, Peyman A. [Survey brain death and organ donation in Iran (Persian)]. Medical Law Journal. 2012; ;6(20):43-54. [Link]
- Iranian Society of Organ Donation. [Global report on organ donation and transplantation 2020 in Iran (Persian)]. Tehran: Iranian Society of Organ Donation; 2020. [Link]
- No Author. Nudging family decision-making process on organ donation. 2019.
- Abbasi P, Yoosefi Lebni J, Nouri P, Ziapour A, Jalali A. The obstacles to organ donation following brain death in Iran: A qualitative study. BMC Medical Ethics. 2020; 21(1):83.[DOI:10.1186/s12910-020-00529-8] [PMID]
- Hejazi SS, Nikbakht S, Jouybari L, Abadi MH, Davoodi D, Azizi TH, et al. Knowledge and attitudes toward brain death and organ donation in Bojnurd. Electronic Physician. 2017; 9(7):4746-52. [DOI:10.19082/4746] [PMID]
- YazdiMoghaddam H, Manzari ZS, Mohammadi E. Nurses’ challenges in caring for an organ donor brain dead patient and their solution strategies: A systematic review. Iranian Journal of Nursing and Midwifery Research. 2020; 25(4):265 -72.[DOI:10.4103/ijnmr.IJNMR_226_18] [PMID]
- AfzalAghaee M, khorsand Vakilzadeh A, Rahmanifar F, Movahed nia N, khaleghi E. [Factors related to organ donation from brain dead patients in teaching hospitals of mashhad university of medical sciences during 1392-1385 (Persian)]. Medical Journal of Mashhad University of Medical Sciences. 2016; 59(3):148-54. [DOI:10.22038/mjms.2016.7715]
- Khoddami Vishteh HR, Ghorbani F, Ghobadi O, Shafaghi Sh, Barbati ME, Rostami Louyeh A, et al. [Causes and follow-up outcomes of brain dead patients in Shahid Beheshti University of Medical Sciences hospitals (Persian)]. Pajoohande. 2010; 15(4):171-8. [Link]
- Hajyhosseinloo M, Eftekhari A, Gorbani S, Zarei A. Study of Brain Death and Organ Donation in West Azerbaijan Province (2004-2010). Iranian Journal of Forensic Medicine. 2011; 17(3):149-55. [Link]
- Heydari ST, Hoseinzadeh A, Ghaffarpasand F, Hedjazi A, Zarenezhad M, Moafian G, et al. Epidemiological characteristics of fatal traffic accidents in Fars province, Iran: A community-based survey. Public Health. 2013; 127(8):704-9. [DOI:10.1016/j.puhe.2013.05.003] [PMID]
- Pourhosein E, Bagherpour F, Latifi M, Pourhosein M, Pourmand G, Namdari F, et al. The influence of socioeconomic factors on deceased organ donation in Iran. Korean Journal of Transplantation. 2022; 36(1):54-60. [DOI:10.4285/kjt.21.0034] [PMID]
- Bahadorimonfared A, Soori H, Mehrabi Y, Delpisheh A, Esmaili A, Salehi M, et al. Trends of fatal road traffic injuries in Iran (2004-2011). Plos One. 2013; 8(5):e65198. [DOI:10.1371/journal.pone.0065198] [PMID]
- Aldawood A, Al Qahtani S, Dabbagh O, Al-Sayyari AA. Organ donation after brain-death: experience over five-years in a tertiary hospital. Saudi Journal of Kidney Diseases and Transplantation : An Official Publication of the Saudi Center for Organ Transplantation, Saudi Arabia. 2007; 18(1):60-4. [PMID]
- Tessmer CS, da Silva AR, Barcellos FC, Araujo CL, da Costa JD, Böhlke M. Do people accept brain death as death? A study in Brazil. Progress in Transplantation . 2007; 17(1):63-7. [DOI:10.1177/152692480701700110] [PMID]
- Desschans B, Evrard P; Coordinator Transplant Section of the Belgian Transplant Society. Organ donation and transplantation statistics in Belgium for 2012 and 2013. Transplantation Proceedings. 2014; 46(9):3124-6. [DOI:10.1016/j.transproceed.2014.09.170] [PMID]
- Mizraji R, Pérez S, Alvarez I. Brain death: epidemiology and quality control of solid organ donor generation. Transplantation Proceedings. 2004; 36(6):1641-4. [DOI:10.1016/j.transproceed.2004.06.066] [PMID]
- Erdoğan O, Yücetin L, Tuncer M, Keçecioğlu N, Gürkan A, Akaydin M, et al. Attitudes and knowledge of Turkish physicians about organ donation and transplantation. Transplantation proceedings. 2002; 34(6):2007-8. [DOI:10.1016/S0041-1345(02)02831-2] [PMID]
- Marks WH, Wagner D, Pearson TC, Orlowski JP, Nelson PW, McGowan JJ, et al. Organ donation and utilization, 1995-2004: entering the collaborative era. American Journal of Transplantation. 2006; 6(5 Pt 2):1101-10. [DOI:10.1111/j.1600-6143.2006.01269.x] [PMID]
Review Paper: Research |
Subject:
Special
Received: 2024/07/11 | Accepted: 2024/11/4 | Published: 2025/07/1
Received: 2024/07/11 | Accepted: 2024/11/4 | Published: 2025/07/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |